
Living with keratoconus, an eye condition keratoconus that affects the cornea, can feel challenging, especially when your vision fluctuates or everyday tasks become more difficult due to distorted vision. But with the right information, insight, and care, you can manage this condition with effective keratoconus treatment and regain clarity and comfort. In this guide, I will walk you through what keratoconus is, how it’s diagnosed and treated, including keratoconus contact lenses, and practical tips for daily life — with support from eye specialists like me, Dr Matt Kauffman at Contemporary Eye Care. For more details about our services, visit our keratoconus treatment page.
Understanding Keratoconus: What Is It?
Keratoconus is an eye disorder in which the cornea, the clear front surface of the eye, thins and bulges into a cone-like shape. This irregular shape distorts vision, causes sensitivity to light, and often leads to frequent changes in prescription. Keratoconus generally begins in early adolescent (teens) and stabilizes in the fourth or fifth decade of life.
Early detection is key, which is why regular monitoring with your eye doctor is essential. Learn more about the diagnosis and management of keratoconus at Johns Hopkins Medicine.
Recognizing the Symptoms
f you suspect you might have keratoconus, watch for:
- Blurred or distorted vision (American Academy of Ophthalmology)
- Sensitivity to light
- Doubling, ghosting, smearing, glare, and/or halos
- Frequent changes in eyeglass or contact lens prescription
- Eye irritation, strain, or a persistent urge to rub your eyes (rubbing can worsen the condition) (AAO)
- In severe cases, sudden corneal swelling (hydrops)
If you notice these symptoms, schedule an evaluation with me at Contemporary Eyecare for professional guidance.
How Keratoconus Is Diagnosed
Diagnosis usually involves several specialized tests:
1. Corneal Tomography – We utilize the most advanced technology (Oculus Pentacam) to diagnose and monitor for the progression of keratoconus.
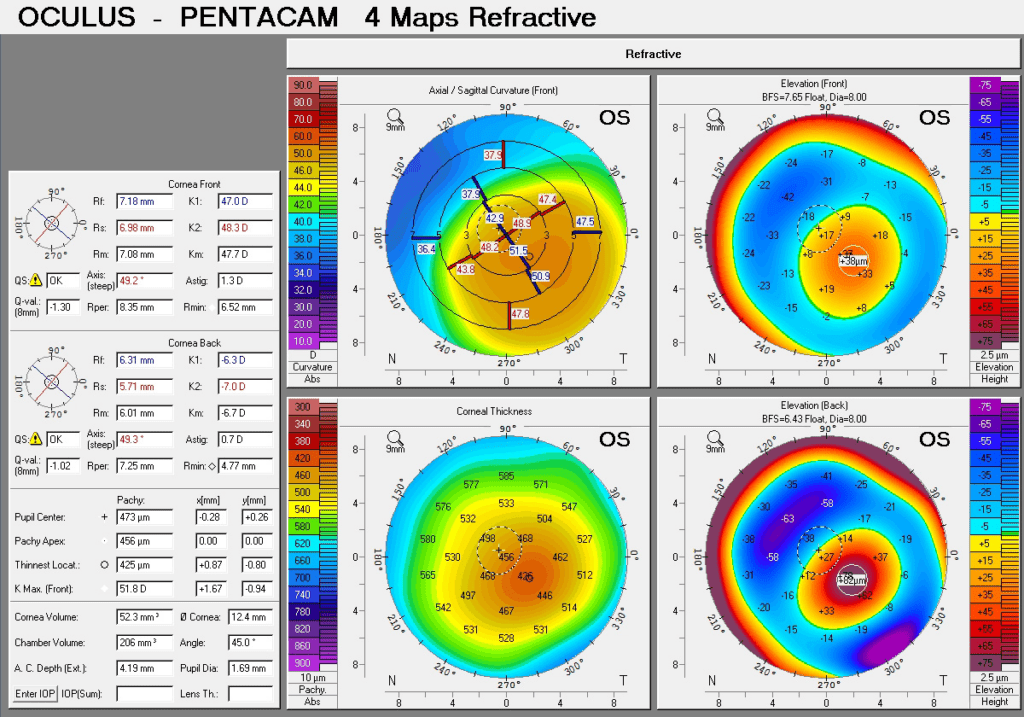
Pentacam corneal tomography display of a patient with keratoconus. The Pentacam is a powerful tool that allows us to detect keratoconus early before it results in significant vision changes.
2. Ovitz aberrometer – Measures higher order aberrations which can result in shadows, doubling, ghosting, or smearing of letters and words
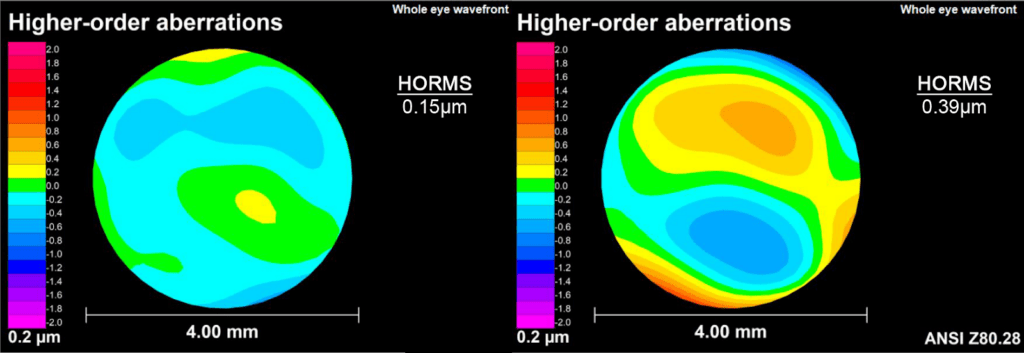
An aberrometer measures higher order aberrations (HOAs), which are distortions that can cause doubling, ghosting, glare, and/or haloes around objects.
3. Zeiss Ocular Coherence Tomographer (OCT) – Provides high definition cross-sectional views of the cornea, which measures the thickness of the cornea.
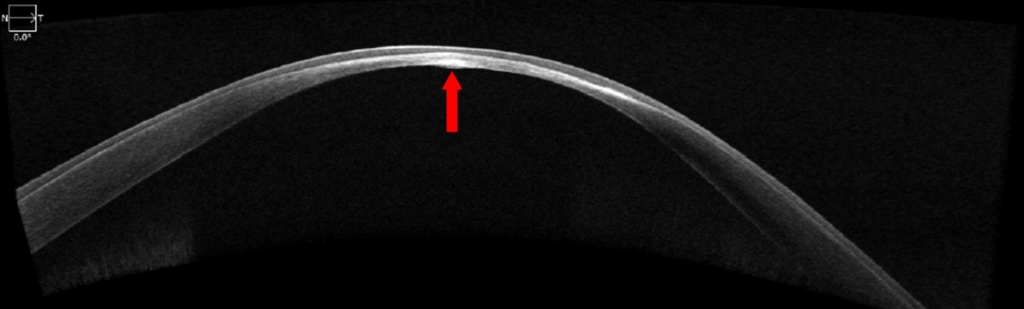
OCT image of a patient with keratoconus. Keratoconus causes the cornea to become more thin, as indicated by the red arrow.
4. Slit-lamp Examination — Microscope exam to detect thinning or scarring (Johns Hopkins Medicine)
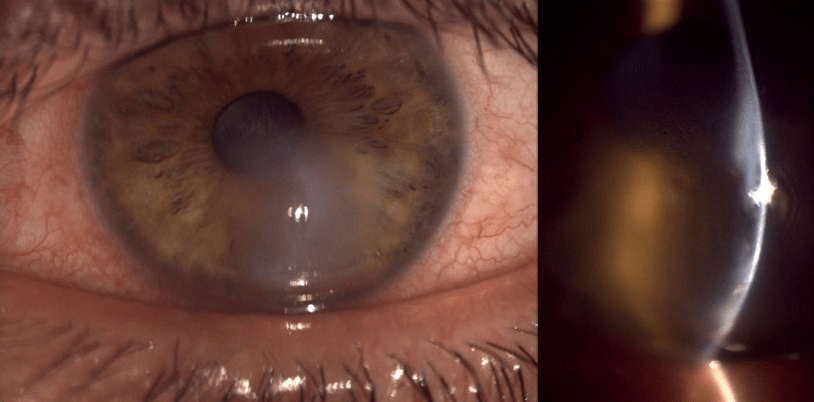
Acute hydrops occurs when the cornea steepens excessively, causing fluid to enter the cornea, which results in blurry vision, redness, pain, and light sensitivity.
Treatment Options: Regaining Clear Vision
Treatment depends on severity and progression. Common options include
1, Optical Treatments
Glasses
Early keratoconus may be corrected with glasses.
For progressing keratoconus, specialized keratoconus contact lenses provide better vision correction than glasses alone:
- Scleral lenses vault over the cornea and provide excellent comfort and vision.
- Wavefront-guided lenses correct higher-order aberrations for sharper vision.
- Rigid gas-permeable or hybrid lenses may also be recommended depending on the corneal shape.
Corneal Collagen Cross-Linking (CXL)
Strengthens the cornea to slow progression
Another emerging option is Corneal Tissue Addition Keratoplasty (CTAK),
which adds donor corneal tissue to improve corneal shape and clarity, potentially enhancing vision for patients with more advanced keratoconus (Vision Institute CTAK).
Intrastromal Ring Segments (Intacs)
Tiny inserts flatten the cornea and improve contact lens fitting (AAO)
Corneal Transplant
Advanced cases may require surgery (Johns Hopkins Medicine)
For detailed information about these treatments, see our Keratoconus Treatment page.
Daily Life Tips
Managing this eye condition keratoconus involves daily habits:
- Avoid rubbing your eyes – Use lubricating drops from Contemporary Eyecare instead
- Regular checkups – Monitor progression with corneal mapping (AAO)
- UV protection – Sunglasses reduce UV damage
- Manage allergies – Reduces eye irritation
- Workspace optimization – Gentle lighting and screen breaks reduce eye strain
Emotional Well-Being
Living with keratoconus can cause stress. Consider:
- Joining support groups or online communities (Keratoconus Group)
- Staying informed – Ask a professional like me, Dr. Kauffman about new treatments and clinical trials
- Setting realistic expectations – Management, not cure, is the goal
When to Contact Your Eye Doctor
Call your provider if you experience:
- Sudden vision changes
- Glare, halos, or discomfort
- Corneal swelling or clouding
Schedule a consultation with Contemporary Eyecare for personalized guidance.
Advances & Research
Recent developments in keratoconus care:
- Smartphone-based screening tools – Early detection (arxiv.org)
- AI & deep learning – Improved diagnosis accuracy (arxiv.org)
Final Thoughts
Keratoconus doesn’t mean giving up on clear vision. With modern keratoconus treatment like scleral lenses, cross-linking, and expert monitoring at Contemporary Eye Care, patients can preserve vision and live confidently despite this eye condition keratoconus and distorted vision.

